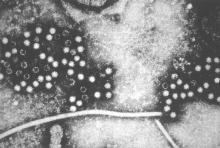
All kidney transplant recipients with abnormal liver function test results should be tested for hepatitis E virus RNA, according to a recent finding by French investigators.
Hepatitis E virus (HEV) is most often transmitted through the fecal-oral route in contaminated drinking water or food, but it also can be transmitted by blood and blood products. A research letter from Dr. Vincent Mallett of the Université Paris Descartes Sorbonne Paris Cité and colleagues published in Annals of Internal Medicine reported a case of HEV transmission to a kidney transplant recipient through plasma exchange.
Nineteen months after a 48-year-old patient received a kidney transplant, Dr. Mallett and his colleagues detected HEV RNA genotype 3f in the patient’s blood based on sequencing, and the patient tested positive for anti-HEV IgG and negative for anti-HEV IgM. The physicians confirmed that the patient had been infected for more than 1 year by finding HEV RNA in a frozen plasma sample drawn 5 months after transplantation. The kidney donor had tested negative for HEV RNA, and the patient’s stored blood samples tested negative for HEV markers before transplantation.
The investigators said that the method of HEV transmission remained undetermined until the investigators tested for HEV RNA in stored samples of all 18 blood products used during the peritransplantation period. From a single sample of fresh frozen plasma from a donor who had tested negative on multiple occasions for hepatitis C virus, HIV-1 and -2, and hepatitis B virus before the plasma was used, the researchers recovered a strain of HEV identical to the one infecting the patient. This plasma had been used during a plasma exchange for treating acute humoral rejection.
Plasma exchange typically involves the removal of 2-5 L of plasma several times a week, Dr. Mallett and associates said, which often is replaced with donor plasma. If replacement involves 2.5 L (10 bags) of donor plasma, which is a typical amount, then the risk for HEV is 10 times greater than the risk involving a single bag.
“In some circumstances, replacement procedures use plasma that has been pooled from many donors and then treated with solvents and detergents to inactivate infectious agents,” they wrote. “However, HEV is not affected by this treatment, so pooling multiplies the risk for infection.”
On the basis of these findings, the coauthors said that “all kidney transplant recipients with abnormal liver function test results, especially those treated with plasma exchange, should be tested for HEV RNA.”
Read the letter in Annals of Internal Medicine (2016 Mar 1. doi: 10.7326/L15-0502).