HISTORY
Lesions on children are the source of much consternation for parents and providers, and understandably so. While the vast majority are safe, there are lesions and conditions that are problematic on a number of levels.
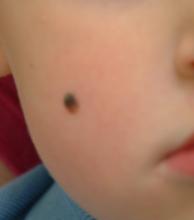
Take this case of a 2½–year-old boy whose parents bring him in for evaluation of the lesion on his cheek. First noticed when the child was an infant, it has grown steadily to its present size (about 5 mm). The child is otherwise healthy, and there is no family history of skin disease or cancer.
The parents indicate their intention to have the lesion removed at the current visit, not realizing what that will actually entail in terms of pain and potential for scarring—not to mention the patient’s willingness to undergo the procedure. All they really know is that the lesion is there, and they want it gone.
On examination, the lesion is papular and black, with some unevenness of color. On palpation, it is firm and nontender, with an apparent intradermal component.
DISCUSSION
This case raises several points—but as to the lesion itself, although it is quite likely safe, it is worrisome, unsightly, and probably “needs to go.”
Based on its appearance and the patient’s age, the lesion probably represents a variant of Spitz tumor, called a Reed tumor or pigmented Spitz tumor. This is a benign lesion that not only resembles melanoma clinically, but also demonstrates microscopic histologic features suggestive of melanoma. Fortunately, it can usually be differentiated from melanoma with special stains and recognition of certain histologic features.
Originally called juvenile melanoma or prepubertal melanoma, these melanocytic nevi were assumed to be malignant; their discovery invariably led to draconian surgical procedures and dire prognoses. In 1947, a Cincinnati pathologist, Dr Sophie Spitz, noticed that none of the “juvenile melanoma” patients she had been involved with had ever shown any signs of cancer. This observation led her to conduct a study of several of these patients, in which it was confirmed that, in fact, these lesions were benign despite their appearance. She went on to determine the histologic differences of these lesions, publishing the results of that work in 1948. It was only after her death at age 46, from colon cancer, that these lesions became known as Spitz tumors, in her honor.
Since then, several variants of this lesion have been described, including the pigmented version described in this case. Another is called spitzoid melanoma—that is, melanoma that demonstrates some of the clinical and histologic features of Spitz tumors but behaves in a malignant fashion. Because of this, and because they mostly occur on children, they are usually removed with modest but definite margins. To this day, differentiation cannot be made on histologic bases alone, adding a significant degree of concern to the diagnosis (although only a tiny percentage ever exhibit malignant behavior).
The more common variety of Spitz tumors, also called epithelioid or spindle cell tumors, are much lighter in color (tan to red to brown) and tend to develop on the face, head, and neck, usually as solitary lesions presenting with an initial phase of rapid growth. The diagnosis of Spitz tumor in an older, sun-damaged patient is considered suspect, with the lesion treated as if it were melanoma.
Besides melanoma, the differential diagnosis for Spitz tumors includes compound nevus, juvenile xanthogranuloma, wart, and basal cell carcinoma.
This patient’s lesion clearly needs excision with clear margins. Given the patient’s age and the location of the lesion, the patient was referred to a plastic surgeon, who in turn will send the specimen to a dermatopathologist experienced in dealing with this tumor.
All this was carefully explained to the family, with reassurance of the probable benignancy of the lesion but also education about the need for continued vigilance. Following surgery, the patient will be followed by dermatology and watched for signs of malignant behavior at the surgical site and in relevant nodal drainage.