HISTORY
A 26-year-old man presents with a lesion on his penis that has existed for many years—at least 10—without significant change and with no attendant symptoms. His new girlfriend, having heard that penile lesions can be dangerous, or even represent contagious disease, insisted that he seek medical evaluation.
He first went to his primary care provider (PCP), who admitted he had no idea what the lesion was; however, he agreed that the longstanding, constant nature of it was reassuring. The PCP advised the patient to consult a urologist. However, the staff at the urology office he contacted advised the patient to consult dermatology instead.
In the dermatology office, a thorough history is taken, including a sexual history that is negative for high-risk factors for HIV or other STDs. Aside from his lesion, the patient has no health-related complaints or causes for concern.
EXAMINATION
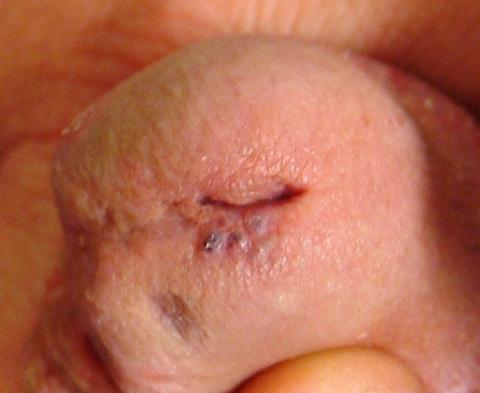
The lesion is actually composed of four grouped purple papules, each about 1 to 1.5 mm in diameter, in aggregate measuring about 8 mm. It is located within 6 mm of the urethral meatus, on the penile glans. The papules are soft and compressible, but barely palpable. Looking elsewhere, no other lesions are seen on the genitals or elsewhere on the body. Notably, the patient is circumcised.
DISCUSSION
I’ve seen these lesions in this exact location several times over a 25-year period. The first was in the early HIV era, and produced enough concern that a biopsy was indicated to rule out things such as Kaposi’s sarcoma or bacillary angiomatosis. What that lesion proved to be is almost certainly what this patient has: angiokeratoma of Fordyce, a totally benign lesion.
These types of angiokeratomas are ectatic, thin-walled vessels in the superficial dermis, with overlying epidermal hyperplasia that forms secondary to normal friction. When they are seen on the scrotum, vulva, or penis, they are usually referred to as angiokeratoma of Fordyce, a type of localized angiokeratoma, other types of which can appear on the legs or hands.
These totally benign lesions must be distinguished from generalized types of angiokeratomata, such as those seen in Fabry disease (angiokeratoma corporis diffusum), an inheritable metabolic disorder. With our patient’s history, his lesion was clearly benign.
Had his lesion been new or changing in any substantive way, additional testing, including a biopsy, might have been necessary to rule out entities such as squamous cell carcinoma (which is almost unknown in circumcised patients), condyloma, melanoma, the aforementioned Kaposi’s sarcoma, or even angiosarcoma.
This case highlights several useful points:
(1) Odd skin lesions need to be sent to the “odd skin lesion” specialist, also known as a dermatology provider. Just because the lesion is on the penis does not mean the patient needs to see a urologist. By the same token, neither does a patient with an odd skin lesion on a foot need to see a podiatrist.
(2) It pays to be a “collector” of anatomic differentials, as in “What lesions might I expect to see on (a given area of the body)?” This concept is valid for any area of the body, and certainly no less true for the penis.
(3) It’s been said that being an effective dermatology provider is as much about “sales” as it is about being an astute diagnostician. In other words, as this case demonstrates, it’s not enough for the provider to be convinced of the identity of the lesion—he must be able to “sell” the concept to a potentially skeptical patient. And in order to do that, the first person he needs to convince is himself.
TAKE-AWAY LEARNING POINTS
• Referral to dermatology is the correct step for any visible lesion or condition, regardless of location—the only exception being internal lesions.
• Just because a lesion is on the penis doesn’t mean it needs to be referred to urology. Skin is skin, irrespective of location.
• It’s not enough to “know” what a given lesion is. Knowing what it isn’t is just as important. And knowing what it means (or doesn’t mean) is often the most important thing of all.
• Anatomic differentials—what types of lesions/conditions are commonly seen in a given anatomic location—are often extremely useful.