Published previously in Gastroenterology (2016;151[1]:40-2).
A 78-year-old man was admitted because of an exacerbation of interstitial pneumonia and was started on steroid therapy. On the next hospital day, he had a stroke. Because of persistent dysphagia, a percutaneous endoscopic gastrostomy tube was placed uneventfully 30 days later.
On hospital day 64, he suddenly developed fever, jaundice, and abdominal distention, followed by hypotension, oliguria, and respiratory failure. Laboratory tests revealed the following: white blood cell count, 44,300/mcL; serum albumin, 2.6 g/dL; aspartate aminotransferase, 1880 U/L; alanine aminotransferase, 1096 U/L; bilirubin, 1.21 mg/dL; and C-reactive protein, 13.5 mg/dL.
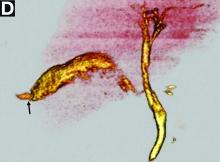
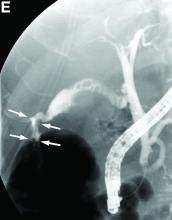
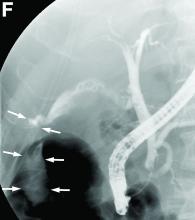
He was diagnosed with septic shock and acute renal failure and was started on continuous hemodiafiltration and mechanical ventilation. Computed tomography (CT) of the abdomen showed marked ascites (Figure A, B), and a diagnostic paracentesis revealed a dark, greenish-brown fluid (Figure C) with a bilirubin level of 14.8 mg/dL.
What is your diagnosis and treatment?