DENVER – Most rashes and other skin conditions are not worrisome, but a few are signs of potentially fatal infections or disease processes.
Recognizing and knowing how best to treat these "death rashes" literally make the difference between life and death, Dr. Heather Murphy-Lavoie said at the annual meeting of the American College of Emergency Physicians.
"You don’t want to miss it. You want to make the diagnosis early and use specific interventions that reduce morbidity and mortality," said Dr. Murphy-Lavoie of Louisiana State University, New Orleans.
She co-created a free app for iPhones and iPads colloquially called "EM Rashes" to help emergency physicians who might be puzzled by a patient with an undifferentiated rash. The app user picks from a selection of rash types, then answers a series of simple questions, such as, "Is the patient febrile?" The app then uses an algorithm to narrow the differential diagnoses, discuss possible causes and findings, and list treatments.
Dr. Murphy-Lavoie offered the following pearls for physicians who are thinking about rashes.
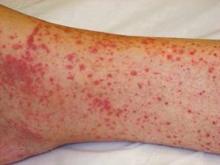
Petechiae and fever? Worry! Only about 50% of people with Rocky Mountain spotted fever will recall a tick bite, so you have to be suspecting it if you’re in an appropriate geographic area. Patients get febrile and toxic. The rash starts out on the wrist and ankle as a maculopapular rash and then spreads and becomes petechial.
"The tip-off is that it spreads to the palms and the soles," she said. "It’s a vasculitis, so it’s a palpable petechiae."
Rocky Mountain spotted fever is a bit of a misnomer, because the disease occurs largely in central and eastern states like North Carolina, Georgia, Tennessee, and Arkansas.
"This is a clinical diagnosis," she said. Don’t wait the 4-5 days it takes to get serology results from a laboratory to decide on treatment. Up to 15% of people with Rocky Mountain spotted fever may develop permanent neurologic deficits. Treatment with doxycycline reduces the risk of death from 30% to 5%. In pregnant women consider chloramphenicol instead of doxycycline, she suggested.
Palpable petechiae, vasculitis could mean infection. A patient with fever, mental status changes, vasculitis, and palpable petechiae should scare you, Dr. Murphy-Lavoie said. This could be meningococcemia, which carries a 3%-50% mortality rate depending on the promptness of treatment. Over the last 10 years in the United States, the mortality has hovered around 13%, she said.
Ceftriaxone is the drug of choice. "Because of diagnostic uncertainty, any time you have a suspected case of bacterial meningitis, you’re going to add on vancomycin to cover resistant Streptococcus," and dexamethasone has been shown to decrease neurologic sequelae, she said. People exposed to a patient with this disease should get prophylactic therapy
Palpable petechiae also are a feature of many types of bacteremia. Petechiae are the most common skin manifestation of bacterial endocarditis, but it’s only present in 20%-40% of cases. When you suspect bacterial endocarditis, get three sets of blood cultures because nailing down the type of bacteria will inform the long-term treatment strategy. Treat initially with broad-spectrum IV antibiotics such as vancomycin and gentamicin to cover methicillin-resistant Staphylococcus aureus (MRSA).
"If you have a S. aureus–related endocarditis, your mortality is almost double that of a streptococcal endocarditis, so you really, really have to make sure that you’re covering for MRSA," she said.
Nonpalpable petechiae = thrombocytopenia. "If petechiae are not palpable, it’s thrombocytopenia unless proven otherwise," Dr. Murphy-Lavoie said.
A febrile, tachycardic woman came to her emergency room complaining of a rash on both legs comprising diffuse, nonpalpable petechiae. She appeared generally ill, had no past medical or medication history of note, and had a very low platelet count. "You should be scared to death if you get this patient in your ER," because she had thrombotic thrombocytopenia purpura (TTP).
More than 90% of patients will die if TTP is not treated with plasmapheresis (also called exchange transfusion), which reduces the mortality risk to 10%. If this treatment is not available at your institution, transfer the patient, she said. Manage the patient in the ICU, and treat the underlying cause of the TTP. Do not give platelets to patients with TTP, which will trigger increased end-organ damage, she warned.
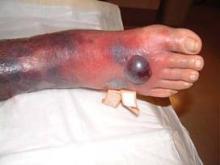
Hemorrhagic bullae? Ominous! "Nothing good causes hemorrhagic bullae," Dr. Murphy-Lavoie said.
Anything that can cause disseminated intravascular coagulation can cause purpura fulminans, which may present with hemorrhagic bullae, rapid hemorrhagic skin necrosis, ecchymosis, purpura, fever, shock, multiorgan failure, and bleeding from multiple sites.