News
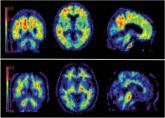

Medicare coverage for amyloid brain imaging should be severely limited, according to a proposed Medicare coverage decision released July 8.
The federal health program proposes to cover only one scan per patient and only as part of a clinical study or to rule out Alzheimer’s disease in narrowly defined and clinically difficult differential diagnoses. The procedure isn’t "reasonable and necessary" otherwise, because there are not enough data to conclude that beta-amyloid imaging with positron emission tomography (PET) improves outcomes for patients with Alzheimer’s disease.
Instead, the Centers for Medicare and Medicaid Services (CMS) proposes to cover the procedure under its Coverage with Evidence Development (CED) program, which provides coverage while collecting additional outcomes data. Coverage under CED contributes to a new technology’s developmental pathway by encouraging more studies that employ it, according to CMS.
Under the draft proposal, PET amyloid imaging would be covered only in CMS-approved, prospective, randomized trials that include subjects from appropriate populations, and, when appropriate, employ the gold standard of postmortem Alzheimer’s diagnosis.
Study populations must comprise Medicare beneficiaries with cognitive impairment suspicious for Alzheimer’s disease, or who may be at risk for developing the disease. Furthermore, studies must address at least one of the following questions:
• Does PET amyloid imaging lead to improved health outcomes, including avoidance of futile treatment or tests; improving or slowing the decline of quality of life; and survival?
• Does treatment guided by PET amyloid imaging identify specific subpopulations, patient characteristics, or differential diagnoses that predict improved health outcomes?
• Can PET amyloid imaging enrich the patient populations of Alzheimer’s trials by selecting patients on the basis of biological as well as clinical and epidemiologic factors? And if so, can this lead to improved health outcomes?
The payment structure will be reconsidered after another evidence review at some unspecified future time, CMS noted.
The draft decision is a disappointment for both patients and the drug companies that are developing amyloid imaging agents. Past CED programs have taken as long as 7 years to return enough evidence for a federal payment reevaluation, according to a statement issued by the Alzheimer’s Association.
"Neither families directly impacted by the disease, nor our federal government, can afford to wait as much as 7 years for a final decision about national coverage, as was the case with the National Oncology Patient Registry and the evaluation by CMS of FDG [fluorodeoxyglucose] PET coverage," the statement said. "The timeframe at which CMS has conducted CED processes is wholly unsuited and unacceptable to both the pace of scientific and technological innovation in the Alzheimer’s field, and more importantly, the rapidly increasing needs posed by the escalating Alzheimer’s epidemic. If the federal government follows this example and timeline, it will hinder coverage of a badly needed, already FDA-approved diagnostic tool in limited populations in which sufficient evidence indicates this technology has meaningful impact."
Avid Radiopharmaceuticals, which manufactures the imaging agent florbetapir F-18 injection (Amyvid), agreed.
"CMS appears to be challenging the value of an adjunctive tool that can assist physicians in making a more informed diagnosis for patients with cognitive impairment," said Dr. Daniel Skovronsky, the company’s president and chief executive officer. "Restricting coverage could hinder a timely and accurate diagnosis, which is in conflict with the advice of Alzheimer’s disease experts and with the administration’s National Alzheimer’s Project Act."
Last January, the Alzheimer’s Association and the Society of Nuclear Medicine and Molecular Imaging (SNMMI) issued revised appropriate use criteria for these agents. Imaging should be reserved for those with persistent or progressive unexplained mild cognitive impairment, MCI that has an atypical presentation, and MCI which develops at an atypically young age, the document maintained.
Imaging was not considered appropriate for asymptomatic patients; for those with typical-onset dementia; as a substitute for risk genotyping in patients with a family history; or to determine dementia severity.
The SNMMI criteria address a small but important patient population not addressed under the CMS proposed payment scheme, said Dr. Richard J. Caselli, professor of neurology at the Mayo Clinic in Scottsdale, Ariz. He also is associate director and clinical core director of Mayo’s Alzheimer’s Disease Center.
"While I can understand the rationale for not reimbursing this in the typical elderly dementia patient, there is another population, albeit smaller, that would clearly benefit: the working patient," he said in an interview. "Imagine a 52-year-old man with no family history, who starts developing memory loss, has trouble on the job as a result, and seeks help. In this case, a diagnosis of Alzheimer’s is unexpected, and will result in disability."


