Do you have a clinical pearl for delivering a deflexed, deeply impacted fetal head at cesarean delivery?
CASE At 2 Am, the director of nursing pages you, asking you to attend to a 26-year-old gravida 1 para 0 who has just been brought by ambulance to labor and delivery after attempting home birth.
The midwife caring for the patient reports that she has been fully dilated for 7 hours and has been pushing for 4 hours. You confirm that the patient is fully dilated, with the presenting part at +1 station; significant caput succedaneum; and molding of the fetal head.
Estimated fetal weight is 3,600 g. The fetal heart-rate tracing is Category II.
You recommend a cesarean delivery. The exhausted patient agrees, reluctantly.
But when you attempt to deliver the fetal head, you realize that it is deflexed and stuck deep in the pelvis. It’s going to be very difficult to deliver the head without trauma to the lower uterine segment, upper vagina and, possibly, the bladder.
What should you do now?
Experienced clinicians often recognize, instinctively, a looming catastrophe before it happens because we have seen a similar situation earlier in our career.1 After we identify the potential for trouble, we attempt to avert disaster by taking preventive action.
One very good occasion to use that “clinical sixth sense”
Consider the situation in which labor has been complicated by a long second stage, with a large fetus—a disaster waiting to happen. In such a case, cesarean delivery, if it is necessary, can be difficult to perform because the fetal head is stuck deep in the pelvis. Attempting to deliver a deeply impacted fetal head, using standard delivery maneuvers, may cause extensive trauma to the lower uterine segment, vagina, and bladder, and fetal injury. In turn, ureteral injury or postpartum hemorrhage may occur during your repair of damage to the lower uterine segment, vagina, or bladder.
In the scenario described a moment ago, the fact that the patient was in the second stage of labor for 7 hours, at home, without anesthesia, and with failure to progress to vaginal delivery increases the likelihood that the fetal head is impacted deep in the pelvis. Before you perform cesarean delivery, you might find it helpful to perform a vaginal examination to answer two questions:
- On vaginal examination, between contractions, can the fetal head be gently moved out of the pelvis? Or is it deeply impacted?
- Is there sufficient space between the fetal head and symphysis pubis to permit delivery with standard cesarean maneuvers?
If the head is impacted deep in the pelvis, I encourage you to consider alternative approaches to cesarean delivery, including reverse breech extraction (FIGURE 1) or an assist from a vaginal hand (FIGURE 2) to facilitate delivery.
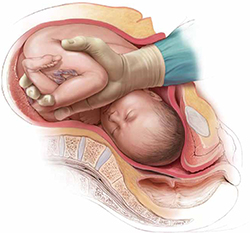
FIGURE 1 Reverse breech extraction—the “pull technique”
Once the uterus has been opened, reach immediately into the upper segment for a fetal leg. Apply gentle traction on the leg until the other leg appears. With two legs held together, deliver (pull) the body of the fetus out of the uterus.
The “pull technique”: Reverse breech extraction
One randomized trial and one retrospective study have evaluated the use of reverse breech extraction (the pull technique) in comparison to pushing up with a vaginal hand from below (the push technique) for managing a difficult cesarean delivery after obstructed labor.
Results of a clinical trial. 108 Nigerian women who had obstructed labor were randomly assigned to a pull technique (reverse breech extraction) or a push technique (assist from a vaginal hand).2
The push technique in this study was reportedly performed with a “finger” in the vagina pushing up on the fetal head while the surgeon attempted to deliver the head in a standard fashion.
The pull technique was performed by opening the uterus, immediately reaching into the upper uterus for a fetal leg, and applying gentle traction on the leg until the second leg appeared. Then, with two legs held together, the body of the fetus was delivered (pulled) out of the uterus. The delivery was then completed using a technique similar to that used for a breech delivery. Standard breech delivery maneuvers were used to assist with the delivery of the fetal shoulders and fetal head.
Comparing the push technique with the pull technique, the push technique was associated with longer operative time (89 minutes compared with 56 minutes [p <.001]); greater blood loss (1,257 mL and 899 mL [p <.001]); and more extensions involving the uterus (30% and 11% [p <.05]) and vagina (17% and 4% [p <.05]) that required surgical repair. The rate of fetal injury was similar using either technique: 6% (push) and 7% (pull).


