Case Letter
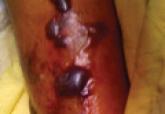
Hemorrhagic Bullous Lesions Due to Bacillus cereus in a Cirrhotic Patient
Traditionally considered in the context of foodborne illness, Bacillus cereus is recognized increasingly as a cause of systemic and local...
Anna H. Chacon, MD
From the University of Maryland Medical Center, Baltimore.
The author reports no conflict of interest.
Correspondence: Anna H. Chacon, MD, 419 W Redwood St, Ste 240, Baltimore, MD 21201 (annachaconmd@gmail.com).

Although dermatology may be regarded as a medical specialty with few emergencies, they do exist and range from primary cutaneous disorders to severe systemic conditions with skin manifestations. Prompt recognition for appropriate diagnosis and treatment often is necessary to improve a patient’s prognosis and a single decision can mark the difference between life and death.
Dermatologic emergency may sound like an oxymoron, but there are many emergencies that dermatology residents may encounter in their careers. In some instances the skin is the primary organ that is affected, while in others cutaneous symptoms and life-threatening signs are important diagnostic clues for what may lie beneath the skin.
As residents who are occasionally on call or on consultation services, it is important for us to recognize dermatologic emergencies quickly because some of these conditions can acutely evolve and become lethal if a diagnosis is not made early in the disease course with the appropriate treatment administered. Dermatologic emergencies can range from severe drug reactions, infections, autoimmune exacerbations, and inflammatory conditions (eg, erythroderma) to environmental insults such as burns (Figure 1) and child abuse.1
Critical Infections
Some dermatologic emergencies are infectious in origin, and although these infections are most commonly bacterial (eg, necrotizing fasciitis), they also can range from viral to fungal (eg, mucormycosis) in nature. Some areas with large populations of immunocompromised patients (eg, human immunodeficiency virus–positive patients, organ transplant recipients) may warrant a high index of suspicion for possible zebras (rare conditions) and opportunistic infections that may quickly escalate to life-threatening situations.
Although few cutaneous manifestations in emergent infections are pathognomonic, they sometimes can be categorized according to the appearance of the primary lesion: erythrodermic (eg, staphylococcal scalded skin syndrome), maculopapular (eg, Lyme disease), purpuric/petechial (eg, Rocky Mountain spotted fever), pustular (eg, disseminated candidiasis), or vesicular (eg, neonatal herpes simplex virus)(Table). On consultations, dermatology residents frequently get called to evaluate hemorrhagic and ischemic lesions in inpatients (Figure 2). Aside from infectious causes, the differential diagnosis may include coagulation abnormalities (eg, concurrent anticoagulant therapies), vasculitides, poisoning, vascular disease, or Stevens-Johnson syndrome and toxic epidermal necrolysis, which can occasionally present with hemorrhagic lesions.1,2
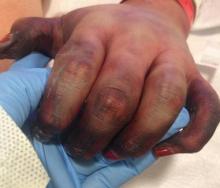 Figure 2. Cutaneous signs of iatrogenic, vasopressor-induced ischemia; gangrene of the distal digits of the left hand; and pronounced demarcation of vessels, as well as a vascular indication of thrombosis and lack of blood flow to the affected areas.
Figure 2. Cutaneous signs of iatrogenic, vasopressor-induced ischemia; gangrene of the distal digits of the left hand; and pronounced demarcation of vessels, as well as a vascular indication of thrombosis and lack of blood flow to the affected areas.
Figure 2. Cutaneous signs of iatrogenic, vasopressor-induced ischemia; gangrene of the distal digits of the left hand; and pronounced demarcation of vessels, as well as a vascular indication of thrombosis and lack of blood flow to the affected areas.

Traditionally considered in the context of foodborne illness, Bacillus cereus is recognized increasingly as a cause of systemic and local...

Orificial tuberculosis (OT) constitutes 2% of cutaneous tuberculosis cases and 0.01% to 1% of all clinical presentations of tuberculosis. It is...

Frostbite is a form of localized tissue injury due to extreme cold that most commonly affects the hands and feet, with the greatest incidence...
