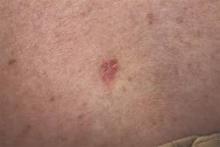
In a small sample study, 10 (36%) of 28 children and young adults diagnosed with nonmelanoma skin cancer were given a misdiagnosis initially, suggesting that young patients with NMSC risk factors may require heightened monitoring from health care providers, according to a study published in Journal of the American Academy of Dermatology (2015 doi: 10.1016/j.jaad.2015.08.007).
In their efforts to identify potential risk factors and gaps in care associated with NMSC in pediatric populations, lead author Hasan Khosravi of Harvard Medical School, Boston, and his associates examined records from 28 patients and 182 occurrences of NMSC, collected from Boston Children’s Hospital between 1993 and 2014.
Thirteen (46%) of the 28 pediatric NMSC patients had a history of prolonged immunosuppression, radiation therapy, chemotherapy, voriconazole use, or a combination of these. Among these 28 patients, 19 were diagnosed with basal cell carcinoma (BCC), 7 were diagnosed with squamous cell carcinoma (SCC), and 2 were diagnosed with both BCC and SCC.
The authors noted significant delays in the initial diagnosis in both types of cancer; the mean number of days from time of lesion onset to diagnosis was 667 for SCC and 1,176 for BCC. When misdiagnosed, carcinomas were incorrectly identified as viral wart and graft-versus-host disease for SCC, and psoriasis, acrochordon, wart, nevus, and atypical nevus for BCC.
Even so, interventions were effective in the pediatric population, the authors noted.
“Although most of our patients developed subsequent NMSC after their initial diagnosis, the majority of cases were treated successfully with surgical excision, without recurrence or spread of disease. This suggests that interventions in children and young adults that involve prevention of subsequent disease may be most impactful,” they wrote.
The researchers had no conflicts to declare.