Article
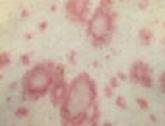
Paraneoplastic Subacute Cutaneous Lupus Erythematosus: An Underrecognized Entity
Subacute cutaneous lupus erythematosus (SCLE) is a form of cutaneous lupus erythematosus that most often presents as scaly, erythematous,...
Dr. Pascucci was from and Drs. Lynch and Fazel are from the Department of Dermatology, University of California Davis School of Medicine, Sacramento. Dr. Pascucci currently is from the Division of Dermatology, University of California Los Angeles.
The authors report no conflict of interest.
Correspondence: Anabella Pascucci, MD, UCLA Dermatology, 514 N Prospect Ave, Redondo Beach, CA 90277 (apascucci@mednet.ucla.edu).

Overlap syndromes are known to occur with connective-tissue diseases (CTDs). Rarely, the overlap occurs at the same tissue site. We report the case of a patient with clinical and histopathologic findings consistent with the presence of discoid lupus erythematosus (DLE) and localized scleroderma within the same lesions. Based on our case and other reported cases in the literature, the following features are common in patients with an overlap of lupus erythematosus (LE) and localized scleroderma: predilection for young women, photodistributed lesions, DLE, linear morphology clinically, and positivity along the dermoepidermal junction on direct immunofluorescence. Most patients showed good response to antimalarials, topical steroids, or systemic steroids.
Practice Points
Although lupus erythematosus (LE) and scleroderma are regarded as 2 distinct entities, there have been multiple cases described in the literature showing an overlap between these 2 disease processes. We report the case of a 60-year-old man with clinical and histopathologic findings consistent with the presence of localized scleroderma and discoid LE (DLE) within the same lesions. We also present a review of the literature and delineate the general patterns of coexistence of these 2 diseases based on our case and other reported cases.
Case Report
A 60-year-old man presented with a progressive pruritic rash on the face, neck, and upper back of approximately 20 to 30 years’ duration. On initial evaluation, the patient was found to have indurated hypopigmented plaques with follicular plugging bilaterally on the cheeks, temples, ears, and upper back (Figure 1). Punch biopsies were performed on the left cheek and upper back. Histopathology was notable for vacuolar interface dermatitis with dermal sclerosis at both sites. Specifically, interface changes, basement membrane thickening, and periadnexal inflammation were present on histopathologic examination from both biopsies supporting a diagnosis of DLE (Figure 2A). However, there also was sclerosis present in the reticular dermis, suggesting a diagnosis of localized scleroderma (Figure 2B). Direct immunofluorescence was negative for a lupus band. Laboratory workup was positive for antinuclear antibody (titer, 1:40; speckled pattern) and anti–Sjögren syndrome antigen A but negative for double-stranded DNA antibody, anti-Smith antibody, anti–Sjögren syndrome antigen B, and Scl-70.
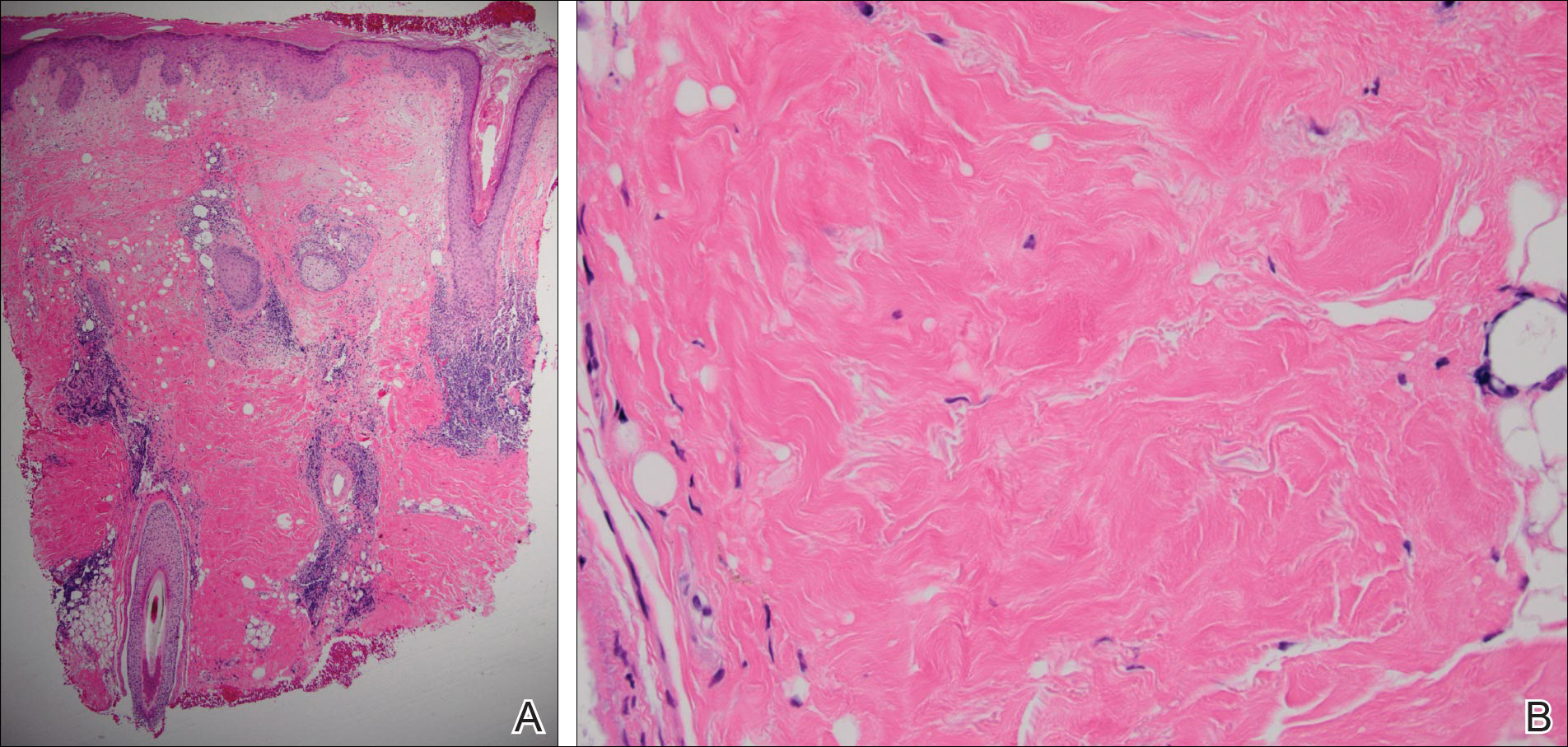
Figure 2. Interface changes, basement membrane thickening, and periadnexal inflammation supporting a diagnosis of discoid lupus erythematosus (A)(H&E, original magnification ×10). Sclerosis of the reticular dermis with thickening of collagen bundles consistent with localized scleroderma also were noted (B)(H&E, original magnification ×40).
The patient was started on oral hydroxychloroquine 200 mg twice daily and clobetasol oint-ment 0.05% twice daily to affected areas. After 2 weeks of treatment, he developed urticaria on the trunk and the hydroxychloroquine was discontinued. He continued using only topical steroids following a regimen of applying clobetasol ointment 0.05% twice daily for 2 weeks, alternating with the use of triamcinolone ointment 0.1% twice daily for 2 weeks with improvement of the pruritus, but the induration and hypopigmentation remained unchanged. Alternative systemic medication was started with mycophenolate mofetil 1 g twice daily. The patient showed remarkable clinical improvement with a decrease in induration and partial resolution of follicular plugging after 4 months of treatment with mycophenolate mofetil in combination with the topical steroid regimen.
Comment
Autoimmune connective-tissue diseases (CTDs) often occur with a wide range of symptoms and signs. Most often patients affected by these diseases can be sorted into one of the named CTDs such as LE, rheumatoid arthritis, scleroderma, polymyositis/dermatomyositis, and Sjögren syndrome. On the other hand, it is widely recognized that patients with one classic autoimmune CTD are likely to possess multiple autoantibodies, and a small number of these patients develop symptoms and/or signs that satisfy the diagnostic criteria of a second autoimmune CTD; these latter patients are said to have an overlap syndrome.1 The development of a second identifiable CTD, hence indicating an overlap syndrome, may occur coincident to the initial CTD or may occur at a different time.1
Essentially all 5 of the CTDs mentioned above have been reported to occur in combination with one another. Most of the reports involving overlap among these 5 CTDs include patients with multiorgan systemic involvement without cutaneous involvement, leading to a fairly simple straightforward classification of overlap syndromes as viewed by rheumatologists.1
When the overlap occurs between the localized forms of scleroderma and purely cutaneous LE, the situation becomes even more complicated, as the skin lesions of the 2 diseases may occur at separate locations or coexistent disease may develop in the same location, as in our case.
More than 100 cases have been reported wherein LE and scleroderma coexist in the same patient.1 Most of these cases have been examples of type 1 overlap (Table 1), though a few have been type 2 overlap, with localized scleroderma coexisting with systemic LE or vice versa.1,2 There are rare reports of an overlap of the localized form of both of these entities (type 3 overlap), as demonstrated in our patient. According to a PubMed search of articles indexed for MEDLINE using the search terms localized scleroderma and morphea as well as discoid lupus erythematosus, we found 12 other cases describing type 3 overlap (Table 2).

Subacute cutaneous lupus erythematosus (SCLE) is a form of cutaneous lupus erythematosus that most often presents as scaly, erythematous,...
Bullous systemic lupus erythematosus (BSLE) is a rare subset of systemic lupus erythematosus (SLE) with bullous lesions in a case fulfilling the...

First-year medical students are faced with the daunting challenge of learning medical terminology, a new language to them. As dermatology...
