Video
All from the Dermatology Service, Memorial Sloan Kettering Cancer Center, New York, New York. Dr. Yélamos also is from the Dermatology Department, Hospital Clínic, Universitat de Barcelona, Spain. Dr. Rossi also is from the Department of Dermatology, Weill Cornell Medical College, New York.
Drs. Hibler, Yélamos, Cordova, Sierra, Nehal, and Rossi report no conflict of interest. Dr. Rajadhyaksha owns equity in and is a former employee of Caliber Imaging & Diagnostics. This research was funded in part through the NIH/NCI Cancer Center Support Grant P30 CA008748 and the Beca Excelencia Fundación Piel Sana (directed to Dr. Yélamos).
The eTable is available in the Appendix in the PDF.
Correspondence: Anthony M. Rossi, MD, Memorial Sloan Kettering Cancer Center, Dermatology Service, 16 E 60th St, Ste 407, New York, NY 10022 (rossia@mskcc.org).

Diagnosis and management of lentigo maligna (LM) and LM melanoma (LMM) is challenging. Novel noninvasive imaging technologies such as reflectance confocal microscopy (RCM) have advanced the ability to better diagnose and monitor challenging lesions. In addition, the new handheld RCM (HRCM) together with the use of videomosaics has allowed an accurate evaluation of large lesions in concave/convex areas of the body (eg, the face). Herein, we review the impact of HRCM in the detection, treatment decision-making, and monitoring of 5 cases of complex facial LM/LMM. In the cases presented, HRCM enabled the detection of subclinical margins, presence of invasion, detection of persistence/recurrence, and monitoring of surgical and nonsurgical therapies. In this preliminary report, our results suggest that HRCM is a versatile ancillary tool in pretreatment decision-making, intraoperative surgical mapping, and posttreatment monitoring of complex facial LM/LMM.
Practice Points
Lentigo maligna (LM) and LM melanoma (LMM) represent diagnostic and therapeutic challenges due to their heterogeneous nature and location on cosmetically sensitive areas. Newer ancillary technologies such as reflectance confocal microscopy (RCM) have helped improve diagnosis and management of these challenging lesions.1,2
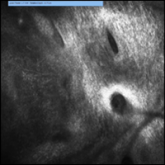
Reflectance confocal microscopy is a noninvasive laser system that provides real-time imaging of the epidermis and dermis with cellular resolution and improves diagnostic accuracy of melanocytic lesions.2,3 Normal melanocytes appear as round bright structures on RCM that are similar in size to surrounding keratinocytes located in the basal layer and regularly distributed around the dermal papillae (junctional nevi) or form regular dense nests in the dermis (intradermal nevi).4,5 In LM/LMM, there may be widespread infiltration of atypical melanocytes invading hair follicles; large, round, pagetoid melanocytes (larger than surrounding keratinocytes); sheets of large atypical cells at the dermoepidermal junction (DEJ); loss of contour in the dermal papillae; and atypical melanocytes invading the dermal papillae.2 Indeed, RCM has good correlation with the degree of histologic atypia and is useful to distinguish between benign nevi, atypical nevi, and melanoma.6 By combining lateral mosaics with vertical stacks, RCM allows 3-dimensional approximation of tumor margins and monitoring of nonsurgical therapies.7,8 The advent of handheld RCM (HRCM) has allowed assessment of large lesions as well as those presenting in difficult locations.9 Furthermore, the generation of videomosaics overcomes the limited field of view of traditional RCM and allows for accurate assessment of large lesions.10
Traditional and handheld RCM have been used to diagnose and map primary LM.1,2,11 Guitera et al2 developed an algorithm using traditional RCM to distinguish benign facial macules and LM. In their training set, they found that when their score resulted in 2 or more points, the sensitivity and specificity to diagnose LM was 85% and 76%, respectively, with an odds ratio of 18.6 for LM. They later applied the algorithm in a test set of 44 benign facial macules and 29 LM and obtained an odds ratio of 60.7 for LM, with sensitivity and specificity rates of 93% and 82%, respectively.2 This algorithm also was tested by Menge et al11 using the HRCM. They found 100% sensitivity and 71% specificity for LM when evaluating 63 equivocal facial lesions. Although these results suggest that RCM can accurately distinguish LM from benign lesions in the primary setting, few reports have studied the impact of HRCM in the recurrent setting and its impact in monitoring treatment of LM.12,13
Herein, we present 5 cases in which HRCM was used to manage complex facial LM/LMM, highlighting its versatility and potential for use in the clinical setting (eTable).




In an article published online on January 26 in the Journal of the American Academy of Dermatology, my colleagues and I (Menge et al)...
