Expert Commentary
Uterus transplantation comes to the United States
The Cleveland Clinic embarks on treating uterine factor infertility
G. David Adamson, MD, and Mary E. Abusief, MD
Dr. Adamson is Founder/CEO of Advanced Reproductive Care, Inc; Adjunct Clinical Professor at Stanford University; and Associate Clinical Professor at the University of California, San Francisco. He is also Medical Director, Assisted Reproductive Technologies Program, Palo Alto Medical Foundation Fertility Physicians of Northern California in Palo Alto and San Jose, California.
Dr. Abusief is a Board-Certified Specialist in Reproductive Endocrinology and Infertility and Chair, Department of Reproductive Endocrine Fertility at Palo Alto Medical Foundation Fertility Physicians of Northern California.
Dr. Adamson reports that he is a consultant to Ferring and has other current financial arrangements with Advanced Reproductive Care, Inc (ARC Fertility) and Ziva. Dr. Abusief reports no financial relationships relevant to this article.

Too many women and men around the world are affected by infertility. Unfortunately, access to assisted reproduction therapies (ART) when necessary is not balanced. These experts address how natural fertility can be optimized and why efforts to address ART access barriers are needed.
In this Article
Patients seeking fertility care commonly ask the physician for advice regarding ways to optimize their conception attempts. While evidence from randomized controlled trials is not available, data from observational studies provide parameters that can inform patient decision making. Knowledge about the fertility window, the decline in fecundability with age, and lifestyle practices that promote conception may be helpful to clinicians and aid in their ability to guide patients.
For those patients who will not achieve conception naturally, assisted reproductive technologies (ART) offer a promising alternative. ART options have improved greatly in effectiveness and safety since Louise Brown was born in 1978. More than 5 million babies have been born globally.1 However, even though the United States is wealthy, access to in vitro fertilization (IVF) is poor relative to many other countries, with not more than 1 in 3 people needing IVF actually receiving the treatment. Understanding the international experience enables physicians to take actions that help increase access for their patients who need IVF.
In this article we not only address ways in which your patients can optimize their natural fertility but also examine this country’s ability to offer ART options when they are needed. Without such examination, fundamental changes in societal attitudes toward infertility and payor attitudes toward reproductive care will not occur, and it is these changes, among others, that can move this country to more equitable ART access.
Factors affecting the probability of conception
Frequency of intercourse impacts the chance of conception. More frequent intercourse results in a higher chance for conception: Daily intercourse results in a 37% chance for conception within a cycle, and intercourse every other day results in a 33% chance for conception. Couples who have intercourse once per week have a 15% chance for conception.4
Frequent ejaculation is not associated with a decrease in male fertility. Results of a study of almost 10,000 semen specimens revealed that, in men with normal semen quality, sperm counts and motility remained normal even with daily ejaculations.5 While abstinence intervals as short as 2 days are associated with normal sperm counts, longer abstinence intervals of 10 days or more may be associated with decreasing semen parameters. It is unclear, however, if this translates into impaired sperm function.6,7
Neither coital position nor postcoital practices (such as a woman remaining supine after intercourse) affect the chance of conception.
Lubricants that do not impair sperm motility, such as canola oil, mineral oil, and hydroxyethylcellulose-base (Pre-Seed) may be helpful for some couples.8 Sexual dysfunction can be a cause of infertility or subfertility. Similarly, stress over lack of conception can impair sexual function; therefore, it is important to ask patients if they experience pain or difficulty with intercourse.
Fecundability refers to the probability of achieving pregnancy within a single menstrual cycle. Studies measuring fecundability reveal that 80% of couples attempting conception will achieve pregnancy within 6 months of attempting and 85% within 12 months. Another 7% to 8% will achieve conception over the next 3 years. The remaining couples will have a very low chance of achieving spontaneous conception.9
The probability of conception is inversely related to female age. Fecundability is decreased by approximately 50% in women who are in their late 30s compared with women in their early 20s.10,11 The chance for conception significantly decreases for women after age 35 and, while the effects of advancing age are most striking for women, some decline in fertility also occurs in men, especially after age 50.11,12
The effects of diet and consumption habits
Folic acid supplementation, at least 400 μg per day, is recommended for all women attempting conception and is associated with a decreased risk of neural tube defects.13 Obese women and thin women have decreased rates of fertility. While healthy dietary practices aimed at normalizing body mass index (BMI) to normal levels may improve reproductive outcomes, there is little evidence that a particular dietary practice or regimen improves conception rates.8 Data are also lacking on the use of fertility supplements to improve ovarian reserve or aid in conception.
Smoking is unequivocally detrimental to female fertility. Women who smoke have been found to have increased rates of infertility and increased risk for miscarriage.14–16 Menopause has been found to occur 1 to 4 years earlier in smoking versus nonsmoking women.17,18
The effect of alcohol on female fertility has not been clearly established, with some studies showing an adverse impact and others showing a possible favorable effect. Based on the available evidence, higher levels of alcohol consumption (>2 drinks/day with 1 drink = 10 g of ethanol) are probably best avoided when attempting conception, but more moderate consumption may be acceptable.8 No safe level of alcohol consumption has been established during pregnancy, and alcohol consumption should be completely avoided during pregnancy.
Caffeine consumption at high levels (>500 mg or 5 cups/day) is associated with impaired fertility. While caffeine intake over 200 mg to 300 mg per day (2−3 cups per day) has been associated with a higher risk for miscarriage, moderate consumption (1−2 cups of coffee per day) has not been associated with a decrease in fertility or with adverse pregnancy outcomes.8,19–22
While the public has access to volumes of information on the Internet, it is important for patients to be educated through accurate information that is best found from professional sources, such as http://www.reproductivefacts.org, offered by the American Society for Reproductive Medicine (ASRM).

The Cleveland Clinic embarks on treating uterine factor infertility
Which patients are likely to benefit from medical therapy? When is surgery indicated? And when is it best to proceed to IVF? Our experts answer...
Although uterus transplantation has been proven to be feasible, is it practical or ethical?
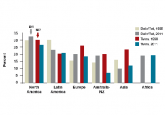
Too many women and men around the world are affected by infertility. Unfortunately, access to assisted reproduction therapies (ART) when necessary...
