PP has an estimated incidence of 1 in 450 pregnancies.11 But while many authorities consider EP to be the most common dermatosis of pregnancy, no clear estimation of its prevalence has been established.23,24 Taken together, these 2 conditions have the highest prevalence of all pregnancy-induced dermatoses. PP is also known as popular dermatitis of Spangler, Nurse’s early prurigo of pregnancy, and linear IgM disease of pregnancy.3,23,25
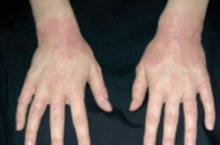
Presentation. The typical presentation consists of grouped, crusted, erythematous papules, patches, and plaques—frequently with excoriations. The lesions typically present on the extensor surfaces of the arms and legs or on the abdomen (FIGURE 4).4 Recurrence in later pregnancies is common.
Pathophysiology. The pathophysiology of EP/PP is not understood. Many patients who present with EP/PP have a history of atopy.10
Differential. Conditions that need to be considered in making the diagnosis include tinea infection, scabies, contact dermatitis, ICP, pruritic folliculitis of pregnancy (PFP), and PG.
Diagnosis. History and physical examination determine the diagnosis. Serology, histopathology, and immunofluorescence are not specific, and correlation with increased IgE is marginal, at best.24,26
Treatment. These conditions are treated symptomatically with topical steroids or systemic antihistamines.
Sequelae. No maternal or fetal increase in morbidity or mortality is associated with these conditions.
FIGURE 4
Eczema of pregnancy
Acute pustular psoriasis of pregnancy
Whether or not APPP is actually a pregnancyinduced dermatosis is subject to debate.
There is evidence that APPP is not unique to pregnancy, but is simply a manifestation of ordinary psoriasis. Clinically and histologically, APPP is indistinguishable from pustular psoriasis. Unlike most cases of acute psoriasis, however, APPP often appears in pregnancy without any personal or family history of psoriasis, and usually ceases when the pregnancy is concluded. This fact, combined with reports of increased fetal and maternal morbidity and mortality associated with APPP, lead us to include it here.27
Presentation. APPP is a rare condition that may have an onset at any point in pregnancy. The characteristic lesions begin as erythematous plaques with pustules on the inner thighs, flexural areas, and groin and spread to the trunk and extremities. As the plaques enlarge, the center becomes eroded and crusted. Nails may become onycholytic. The hands, feet, and face are usually spared. Oral and esophageal erosions can occur. Pruritus is typically mild, although the lesions are often painful and flu-like symptoms are often present.28
Pathophysiology. The pathophysiology of this disease is unknown.
Differential. Conditions with similar presentations include an adverse drug reaction, pityriasis rosea, lichen simplex chronicus, eczema, lupus, and pityriasis rubra pilaris.
Diagnosis. Clinical history and association with systemic illness are the basis for a diagnosis of APPP. Cultures of the pustules are negative for any infective pathology, though as the disease progresses, pustules may become superinfected. Lab tests may show an increased erythrocyte sedimentation rate (ESR), hypocalcemia, and low levels of vitamin D.
Treatment. Prednisone 15 to 60 mg per day is often sufficient to control the disease.28 Cyclosporine 100 mg twice daily has also been shown to be useful.29 Cyclosporine in pregnancy is a category C drug. Data on fetal malformation associated with cyclosporine therapy are limited, but the risk appears to be minimal.6 Maternal hypocalcemia should be monitored and treated appropriately. If disease progression is judged serious enough, early induction of labor is indicated, since delivery will almost always lead to swift resolution.
Sequelae. There have been a number of case reports that link APPP to serious sequelae, including fetal growth retardation, hypocalcemia, and stillbirth.28,30,31 The condition is too rare, however, for good data on specific sequelae. While the disease does give significant cause for concern, it would appear that some of the traditional apprehension comes from older publications reporting a rate of maternal mortality of 70% to 90%.32 This statistic has not been borne out in clinical practice. It does appear that the mother will frequently suffer from systemic symptoms, including fever and malaise.
Pruritic folliculitis of pregnancy
Accounts of PFP’s prevalence vary widely: Some sources report fewer than 30 cases in all of the literature, while others indicate that the prevalence is equivalent to that of PG, 1 in 10,000.3,11 PFP most commonly presents in the third trimester. It often resolves before delivery, but uniformly clears within 2 weeks of delivery.
Presentation. PFP presents as papules and pustules concentrated around hair follicles (FIGURE 5). Often lesions begin on the abdomen and spread to the extremities.24,29 The condition is often, but not always, pruritic. Patients are more likely to be concerned about what the condition means for their health, rather than being distressed by the symptoms.