Ensure that all newborns undergo pulse oximetry screening before discharge—and that abnormal results are immediately followed up with echocardiography.1
STRENGTH OF RECOMMENDATION
B: Based on a single cohort study consistent with multiple studies in other populations.
Ewer AK, Middleton LJ, Furmston AT, et al. Pulse oximetry screening for congenital heart defects in newborn infants (PulseOx): a test accuracy study. Lancet. 2011;378:785-794.
ILLUSTRATIVE CASE
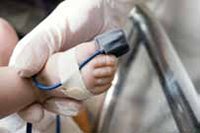
A healthy, full-term baby is admitted to the newborn nursery. Antenatal surveillance, including routine ultrasound, was normal, as are physical examinations, both on admittance to the nursery and on the following day. Should the infant undergo pulse oximetry screening prior to discharge?
Congenital heart defects (CHD) are a leading cause of infant deaths in the developed world, occurring in approximately 9 of every 1000 live births.2 Roughly a quarter of those affected will have CHD serious enough to require either surgery or catheterization within the first year of life. These newborns are susceptible to sudden cardiovascular collapse due to changes in pulmonary vascular resistance and closure of the ductus arteriosus2—changes that often occur after the babies have gone home.
Delayed diagnosis is linked to worsening disease
A study evaluating 286 neonates admitted for cardiac surgery found that delayed diagnosis of CHD was associated with a worse preoperative condition. Cardiovascular compromise and end-organ dysfunction were most common in infants who presented with symptoms after they had gone home, the researchers found.3
In the past, screening for CHD hinged on mid-trimester ultrasound and postnatal physical examination. However, these methods do not reliably detect the condition in a timely fashion.4,5 More recently, pulse oximetry has been used for screening.
International studies prompt US recommendation
In a prospective multicenter trial in Saxony, Germany, more than 41,000 infants born between 2006 and 2008 underwent pulse oximetry screening at 24 to 72 hours of life.5 If the oxygen saturation was ≤95% and confirmed an hour later, echocardiography was performed. Pulse oximetry screening yielded true-positive results in 14 cases, false-positive results in 40, and false-negative results in 4. Sensitivity and specificity were 77.8% and 99.9%, respectively.
In another German study, 3364 term neonates underwent pulse oximetry screening between 6 and 36 hours of life.6 Eighteen neonates (0.5%) had abnormal results, 9 (50%) of whom were found to have heart defects. In this study, pulse oximetry had a sensitivity of 82% and a specificity of 99.9%.
A cohort study of 39,821 newborns in a single region of Sweden found that combining physical examination with pulse oximetry screening had a sensitivity of 82.8% and a specificity of 98%.7 No infants who underwent screening died from undiagnosed ductus arteriosus-dependent lung circulation, compared with 5 such deaths in regions where pulse oximetry screening was not done.
Encouraged by these findings, in late 2011 the US Secretary of Health and Human Services, with strong backing from the American Academy of Pediatrics, recommended universal pulse oximetry screening to detect critical CHD.8 The study detailed below took another look at its efficacy.
STUDY SUMMARY: Detection rate is higher for critical heart defects
The cohort study by Ewer et al enrolled 20,055 neonates born at >34 weeks’ gestation.1 All were screened with pulse oximetry on the right hand and on either foot and had a physical exam within their first 24 hours (The TABLE describes the screening protocol). Infants with a normal pulse oximetry and normal clinical exam were followed for a year to identify late-presenting heart defects.
One hundred ninety-five of the neonates who were screened had abnormal pulse oximetry test results; of these, 26 (13%) were found to have either critical (requiring intervention <28 days) or major (requiring intervention <12 months of age) CHD. Of the 169 infants who had positive pulse oximetry results but did not have critical or major heart defects, 6 were found to have less serious heart defects and 40 had infective or respiratory disorders that also required medical intervention.
Among the 19,860 infants with normal pulse oximetry, 27 (0.1%) were found to have either critical or major heart defects.
Pulse oximetry had a sensitivity of 75% (95% confidence interval [CI], 53.3-90.2) and a specificity of 99.1% (95% CI, 98.98-99.24) for detecting critical CHD. Sensitivity of pulse oximetry for all major CHD was 49% (95% CI, 35.0-63.2) and the specificity was 99.2% (95% CI, 99.02-99.28). The specificity may have been better if screening had been done after 24 hours of life; as seen in other studies,5,6 screening within the first 24 hours leads to more false-positive results.

